Adjusting the Prescription
The School of Medicine overhauls its century-old educational approach

When the Claude Moore Medical Education Building emerged from the construction rubble in 2010, it was apparent that the rules were changing. Set among all the square profiles and institutional red brick of the UVA Health System complex, its round structure of glinting glass looked, from the outside, less like a building than some futuristic beehive.
It signifies a huge culture change within the School of Medicine. After the ritual white-coat ceremony at the start of the fall semester, the Class of 2014 entered a brave new world: They would be the first group to try a different curriculum, test the facility’s innovative educational technology and undergo a learning experience unlike that of previous generations. After four years, they are expected to graduate with the habits of mind—curiosity, skepticism, compassion, wonder—that will prepare them to be better physicians.
Like medical schools across the country, UVA has been undergoing a serious self-examination. Despite transformations in medical science and how it is practiced, the fundamental structure of medical education had not changed in a century. Most universities continue to follow a blueprint introduced in 1910, which called for two years of in-depth study of the basic sciences followed by two years of clinical experience. A cookie-cutter approach, it means that students spend two years sitting through long lectures and regurgitating facts on tests, followed by the shock treatment in their third year of suddenly dealing with patients in a hospital ward.
About half of all medical knowledge becomes obsolete every five years. Every 15 years, the world’s body of scientific literature doubles. The pace of change has only accelerated.
“It’s become pretty clear in the last couple of decades that this is probably not the best way to learn something as complex as medicine,” says Randolph Canterbury, the medical school’s senior associate dean for education. “The idea that physicians ought to learn the facts of all these various disciplines—anatomy, physiology, biochemistry and so forth—to the depth that we once thought they should doesn’t make much sense.”
About half of all medical knowledge becomes obsolete every five years. Every 15 years, the world’s body of scientific literature doubles. The pace of change has only accelerated. “The half-life of what I learned in medical school was much longer than what it is today,” adds Canterbury, a professor of psychiatric medicine and internal medicine.
Armistead Talman (Col class of ’54, Med class of ’58), a retired general surgeon, recalls his first two years of medical school as particularly tedious—to the extent that he wondered whether he should have transferred to the Law School. “The lectures were well done, but it was just that it was so repetitious in terms of the curriculum,” he says. “We kept getting told that eventually it all would have some meaning with respect to clinical application, but that seemed a fairly abstract statement.”
A study last year by the Carnegie Foundation for the Advancement of Teaching criticized present-day medical education as “inflexible, excessively long and not learner-centered.” It called for a range of broad reforms aimed at improving the quality of physician training, including a better integration of formal knowledge and clinical experience and a learning process that is individualized, not one-size-fits-all.
Within the School of Medicine, all of these pressures led to something of a perfect storm. As plans advanced for the new $40.7 million building—it was the only school at UVA without a dedicated teaching facility—it coalesced into an unusual, functionally innovative design, one built around a new pedagogy.
Clearly, the prospect of a new approach was a draw for many students. The percentage of students who accepted offers of admission for fall 2010 set a record high.

Learning in the round
On this December morning, the low rumble of conversation in the “learning studio” gives an illusion that class hasn’t started; after all, there’s no sign of a professor at the lectern. In a 4,500-square-foot circular room, 155 first-year medical students sit at round tables arrayed with their laptops and fuel for the next few hours: insulated coffee mugs, bananas, Ziploc bags of homemade cookies. This week’s theme, “Tolerance and Immunization,” is part of a semester-long course in molecular and cellular medicine. Instead of separate classes in four or more different disciplines, the curriculum is synthesized, interweaving clinical issues with the basic sciences.
In teams of eight, the students debate a patient case: Walt Z., a 55-year-old chemist, comes into your clinic complaining of intermittent chest pain. As his doctor, you’ve arranged for an exercise stress test. But Walt Z. is an informed consumer of health care, and he has lots of questions about the test’s accuracy in diagnosing blockage in coronary arteries. Five large media screens hanging throughout the room delineate his medical details and a series of multiple choice questions.
Gone is the traditional 50-minute lecture. (Also gone is paper, for the most part.) The students have completed the assigned reading beforehand and, because they’ve absorbed the facts on their own, class time serves another purpose. Self-assessment tests at the start of class measure how well they understand the material. Then it’s time to do a test case, to reinforce their critical thinking and push their knowledge and skills to another level.
“We are tying things together clinically, giving them insight into how it fits in with the patients,” says Linda Waggoner-Fountain, an associate professor of pediatrics and co-leader of the fall semester’s molecular and cellular medicine course. “The skills are more immediately applicable. In adult learning theory, this is the goal: to apply your knowledge right away.”
The course leader, Denise Bonds, an associate professor in the Department of Public Health Services, appears at the center of the room to lead the next phase of the discussion. The room’s interactive technology allows her to link to students’ laptops; it also enables their work to be broadcast onto the big screens. Instead of a blackboard, she can use a document camera, which is like an overhead projector, allowing her to write or draw a diagram that will project on the screens. Absentees can view a podcast of the session.
In this “flattened classroom,” as it’s been described, the traditional top-down educational approach is reconfigured and the responsibility for learning shifts to the student.
Students at each table have reached a consensus on the case, maybe having done some research online. Bonds calls out “Survey says?” and a member at each table raises a laminated card with their answer (A, B, C or D). Bonds points to a table and its spokesperson takes the built-in mic to defend their answer. She then gives a short, focused lecture, which is followed by a discussion about the difference between a test’s sensitivity and its specificity and the questions that arise in determining what test for Walt Z. is most accurate.
Problem solving by teams mirrors the reality of health care today. “The traditional approach has been one patient, one doctor,” says Waggoner-Fountain. “Now, it’s one patient, one doctor and a team, in part because medicine has gotten more sophisticated and patient expectations are different.”
Studies also show that individual grades improve when working within a team. The first-year students have embraced it. Not isolated in auditorium seats bolted to the floor, they can easily move and mingle because everything is in the round.
“Working in a team reinforces what you learn in class,” says Chelsea Becker (Med class of ’14). “We all have different backgrounds and everyone knows something different.” Science majors don’t hold dominion; the class comprises more than 60 different majors, from astrochemistry to art.
“It allows us to teach each other,” adds Tom Jenkins (Med class of ’14), who estimates he’s collaborated with just about every person in the class at this point. “I think that helps with retention.”
Practicing early, and often
Medical simulation is another way of aiding retention—particularly when it’s orchestrated to be stressful.
“You want the learner to be stressed enough to make this relevant and important to them, and to re-create the emotions that they are going to feel when they have to take care of a patient, especially in a crisis situation, without scaring them so much that they are disabled,” says Keith Littlewood, an associate professor of anesthesiology and co-director of UVA’s Medical Simulation Center.
UVa Medical Center's Medical Simulation Center from UVA Magazine on Vimeo.
The retooled curriculum promised beginning students more hands-on learning, but perhaps a lot sooner than they anticipated—in their second week. Since each student entered medical school certified in emergency life support, Littlewood created a mock scenario involving a couple of patients suffering cardiac arrest. “We’re trying to create a situation in which they are thinking as a physician working with a patient, not as a professional test taker,” he explains, “which is kind of what they are when they come here, through no fault of their own.”
Simulation has emerged as essential to medical education and assessment. It creates a safe environment to make mistakes and think through what went wrong. It’s hugely popular with medical students, residents and clinicians alike. But until now, first-years have never experienced this component.
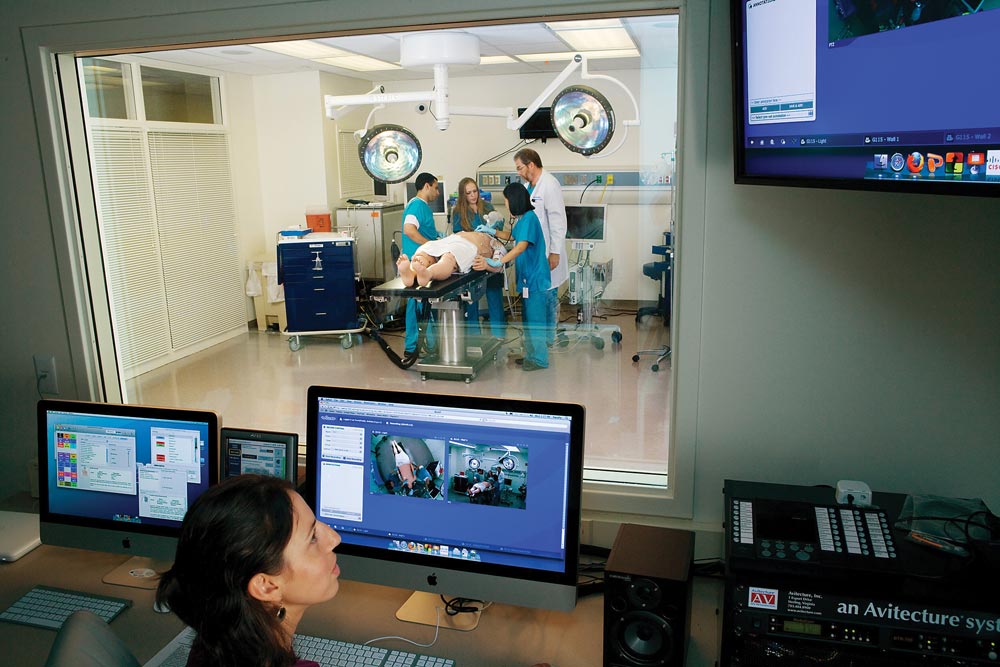
Occupying an entire floor in the new building, the simulation center moved from a cramped 1,200-square-foot space in the Old Hospital to more than 10,000 square feet. Four large simulation rooms—an operating room, emergency room, intensive care unit and labor and delivery room—offer an array of realistic scenarios. There are also six procedure rooms for skills workshops, a faux emergency vehicle entrance at the building’s rear plus a triage area and decontamination bay.
What makes UVA’s simulation center unique nationally is its primary focus on educating medical students.
The school’s pride and joy might be the eight sophisticated patient simulators (six adult, two pediatric). Its high-end simulator, a $250,000 model, is a feat of engineering. It blinks, breathes and has a pulse. It can be put to sleep just like a person. Technologists on the other side of a one-way mirror manipulate its vital signs. Perhaps their most powerful tool is being able to assume the voice of the patient. Experienced clinicians who skeptically enter a simulation room—“walking in and seeing a big Ken doll on a stretcher,” Littlewood says—quickly suspend their disbelief when it suddenly moans and demands to know what’s going on.
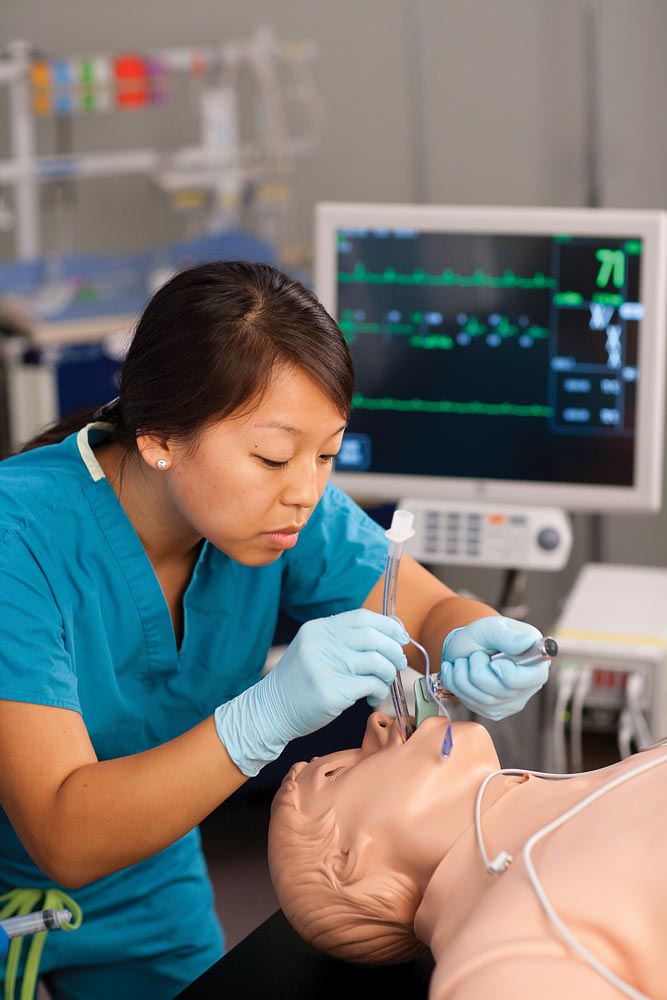
As impressive as the staging of a simulation is, the real educational impact occurs during debriefing. Five cameras positioned throughout the room have recorded everything, including the patient’s monitor information. Immediately following the exercise, students move to a separate room where, still highly energized, they watch the video and reflect on their decision making as physicians in that particular situation.
“Debriefing, to me, is a fascinating area,” says Mark Kirk, an associate professor of emergency medicine and pediatrics and co-director of the simulation center. “You facilitate the discussion, but really you’re trying to get the group to talk. The questions I ask are: ‘What were you thinking? What information were you trying to gather?’”
When students see themselves on video, they have a much better understanding of who they are and what they appear to be. Sometimes there’s an uncomfortable disconnect between the two.
The cardiac arrest scenario was repeated 26 times, for groups of six students. There were no defined roles or forewarning of what they would be tested on. Every team experience was singular. “We have the sense that education should be standardized and everyone should have the same experience, but that’s not really the case for us,” says Littlewood. “The new Carnegie report talks about having standardized outcomes for individualized experiences, and I think there’s no better example than over here.”
On another floor of the new building, the Clinical Skills Center adds a human element. Here, students can refine their cognitive and psychomotor skills but also develop the talents for listening and communicating that will serve them well as physicians. The school has trained about 150 actors to simulate a variety of symptoms and diseases, all drawn from actual cases. Students interview these “standardized patients,” take their medical histories and examine them in 16 outpatient and four inpatient procedure rooms. At computer work spaces outside the rooms, the students chart their evaluations. As culturally diverse as patient populations tend to be, the actors provide immediate feedback, assessing not only diagnostic ability but also “bedside manner.” Unlike their predecessors, this class will practice such skills earlier and more often.
Education 101
Concepts like “active learning” don’t sound new because they aren’t—except perhaps in the first phase of medical education.
“Doctors have not been trained as educators,” says Susan Pollart (Med class of ’82), associate dean for faculty development and an associate professor of family medicine. Learning theory might as well be a foreign language. “That is changing now. But by and large, they haven’t learned how to teach.”
By the standards of Bloom’s Taxonomy, a hierarchical classification system that formulates six levels of cognitive skills, the first two years of traditional medical education has been stuck near the bottom, according to Pollart. Knowledge of basic facts occupies the lowest rung; then the rungs move up through comprehension, application, analysis and synthesis to creation at the top.
Faculty have always informed the next generation in the same way that they were: the time-honored didactic manner. With so many advanced tools in the new facility, however, they now have the opportunity to change the game.
First, some uncomfortable truths. Lectures have largely become outmoded; at most medical schools, they are no longer mandatory and reportedly less than 50 percent of students attend them. Some studies indicate that students can master the same amount of content in a third less time using computer-assisted learning. Other studies in modern learning theory indicate that hour-long lectures are not the best way to teach students because the average attention span for listening to one is about 12 minutes.
In late 2009, Pollart began organizing workshops that brought in consultants and educational experts to help faculty with the basics, like establishing learning objectives and outcomes in this newly integrated, interactive curriculum. A faculty journal club continues to meet biweekly to discuss topics relating to best practices in education.
The circular learning studio, Pollart notes, is designed for learning, not teaching. Professors were unsure how to use it to their best advantage. There were awkward physical challenges. If the room has no front or rear, where do they stand? If they circulate among the tables, how do they change material on the screens? In the new space, they’ve practiced their movements like actors block a play.
Faculty have adapted to the new approaches at different rates. There was some initial resistance. Some faculty felt a little offended, says Canterbury. “They’ve given lectures they’ve gotten praise for doing, for which they’ve gotten wonderful evaluations from students,” he says, “and now we’re saying, ‘You’re really good at doing that, but that’s not what we want you to do anymore.’ That’s a hard thing to do.”
The goal this year is for 40 percent of the classes to have an active-engagement format. Next year, the goal is 50 percent. While they haven’t met the initial goal, “the light bulb has definitely gone on,” Pollart says. “Now, it’s gotten people excited.”
For that, the faculty may have the students to thank. In the learning studio, they clap at the end of every session. At the conclusion of the fall semester, they uncorked champagne (nonalcoholic) and presented flowers to their instructors.
The fall semester was one long experiment. Faculty tried many new things, Canterbury says, and some approaches worked while others fell flat. There have been some technical bugs with the newly installed technology. Mostly, though, it went well and students were forgiving of the glitches.
“It’s such a big thing, this curriculum, to totally restructure it. It’s hard for them to make on-the-fly changes from feedback sometimes,” says first-year medical student Tom Jenkins. Elected at the beginning of the term as a student liaison to the administration, he shares the concerns of his fellow students at weekly evaluation sessions. “The faculty really wants us to understand, not parrot back a lot of rote information, which I think is excellent,” he adds. “I like the way everything meshes. I’m intrigued by the new technology; when it works, it works really well.”
New accrediting standards from the Liaison Committee on Medical Education make it critical for UVA to complete this process of retooling the curriculum. Alumni like Armistead Talman—whose class gave more than $1 million toward the facility at its 50th reunion—foresee a more stimulating and patient-oriented introduction to what he calls “the complexities and wonders of medicine.”
Jenkins says his friends attending medical school elsewhere “feel like they are showing up to a dark room for four to six hours a day, sitting through lectures and PowerPoint slides.” In contrast, he and his UVA classmates say they are more engaged and less stressed—a good barometer of the program’s success so far.

