Once and Future Plague
Coming to grips with a pandemic
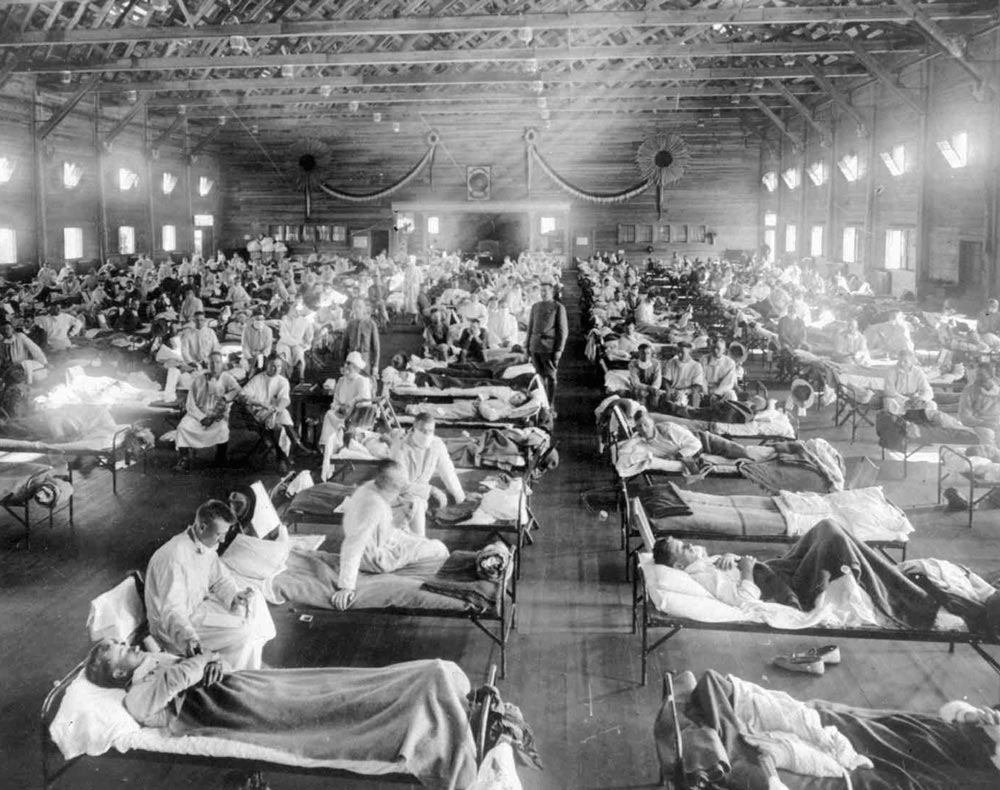
It’s the kind of math that terrifies.
Forty million to 50 million deaths, 675,000 in the U.S. alone. The average American lifespan cut by a dozen years. Nearly 10 percent of the world’s young people died in 1918. And from what disease? The flu. It’s a gnat-sized word that has hardly chilled us in recent years, even while conventional influenza kills a million people annually. And most of us don’t get vaccinated.
But in 1918, “flu” meant “plague.” In his 2004 book, The Great Influenza, author John Barry reports that an intensely virulent strain of Influenza A killed more people in 24 weeks than AIDS has killed in 24 years, more in a year than the Black Death in a century. Most deaths were sudden and severe—fever, joint pain and piercing headaches afflicted victims who often died in just days. Despite the staggering death toll, many people draw a blank when asked about the 1918 pandemic. Movies and recollections of high school history class may help us conjure the distant faces of World War I figures like “Black Jack” Pershing or the Red Baron, but we scratch our heads when trying to recall anything specific about the most lethal outbreak of illness in history.
As Jeffrey Olick, a UVA sociology professor and a specialist in collective memory, notes: “People have a general sense that some time a while ago there was a really bad flu epidemic.” But those memories blur, he says, into a general epidemiological dread—an admixture, perhaps, of early AIDS hysteria, the SARS panic, the encephalitis scare in New York City in 1999, and even Biblical plague terrors that linger in the collective unconscious.
But for some scientists, the year 1918 yet thunders: they see the date in italic boldface. It’s as close as we can get to imagining the next pandemic—one we are on the brink of, according to the World Health Organization.
At the University of Virginia, medical experts and professionals in diverse fields are wrestling not only with the public health implications of a possible pandemic, but with the potential ethical, societal and economic effects. Among those on the front lines of the emerging global threat is Dr. Frederick Hayden, an avian flu expert and UVA professor of internal medicine and pathology. This past fall, in the New England Journal of Medicine, Hayden and an international team of physicians issued clinical guidelines for detecting and containing transmission of H5N1, the deadly avian flu virus that continues to circulate in Asia.
Hayden spelled out a probable future in a recent talk at UVA’s Miller Center of Public Affairs. “We can anticipate a viral disease affecting individuals on a worldwide basis across the age spectrum,” he says. “First there has to be the appearance of a novel Influenza A virus for which the population possesses little or no immunity. It has to be a virus that can infect individuals and cause disease in them. And a key element would be the ability of the virus to transmit from one person to another.” While it has yet to manifest the capacity for easy human-to-human transmission, avian flu otherwise fits the bill. “And that’s why there’s such a concern about a threat of pandemic influenza,” he adds.
Even if a pandemic doesn’t strike anytime soon, it seems that the fear of one has become part of our contemporary outlook. Perhaps that fear is just the strident edge of a necessary wake-up call. “We as a country haven’t paid enough attention to the threat of both seasonal and pandemic influenza,” says Hayden.
Hayden has been working with the WHO and researchers in Southeast Asia to conduct clinical trials on several new antiviral drugs for the flu, a stopgap measure until an effective vaccine can be developed.

The Human Toll
As of late January, some 200 avian flu cases and 83 deaths had been reported in Vietnam, Thailand, Indonesia, China and Cambodia; as the year began, Turkey charted four fatalities and on Jan. 29, European Union authorities detected the presence of H5N1 in poultry in Cyprus. More than 100 million chickens have been killed by the virus or in attempts to control it. H5N1 has as its reservoir the world’s migratory wildfowl. It can be passed to domestic poultry, as it has in Southeast Asia’s myriad markets and farms. And, albeit rarely, its genes can seep into those smaller pools of Influenza A viruses that infect people.
In reconstructing the 1918 virus, Jeffrey Taubenberger of the Armed Forces Institute of Pathology found that the virus was an avian strain that had mutated sufficiently to readily infect humans. Luckily, the most recent strain, a cousin to a 1997 virus detected in Hong Kong, hasn’t yet shown that capacity. But it could mutate, and that mutation could spark a pandemic.
Should that occur, the math, once again, would be devastating. While early fear-mongering has subsided (ABC’s Frontline initially reported 1 billion possible deaths), the latest speculation isn’t reassuring. Mike Leavitt, secretary of the U.S. Department of Health and Human Services, warns that a virus issuing from bird flu “could become one of the most terrible threats to life that this world has ever faced.”
To date, the estimated potential worldwide death toll ranges from 7.4 million to 180 million to 360 million, extrapolating 1918’s deaths to today’s population. Given global air travel, the virus could spread swiftly, possibly reaching all continents in three months, the WHO asserts. The federal government fears that 9 million Americans may become sick; most experts now assess the potential mortality rate at 1.5 percent to 2 percent. An index of how overtaxed health-care resources might become is the Centers for Disease Control and Prevention’s estimate of roughly 200 million outpatient visits and 2 million to 5 million hospital admissions.
Aside from medical costs, the social and financial repercussions could be staggering, with global preparedness woefully inadequate. “Despite the certainty of a pandemic, even developed countries are unprepared, public health infrastructure is inadequate, hospitals lack the capacity to accommodate a surge of patients and the repertoire of antiviral drugs is completely inadequate,” Hayden notes.
In mid-January, a major vaccine manufacturer began producing a shot to protect humans against bird flu. It’s part of the federal government’s $4 billion plan to combat a pandemic. But whether that plan is viable remains questionable. The new vaccine may not be effective if the virus mutates. Even if it works, it’s highly unlikely that the supply will be sufficient. According to the Department of Health and Human Services, it will take until 2009 to stockpile enough vaccine for 20 million people; 2010 is the target date for the drug industry to be able to build enough capacity to deliver emergency production.
While osteltamivir and zanamivir, the major antivirals, do a good job of alleviating symptoms, we don’t have enough of them, either. The U.S. stockpile of 2.3 million courses of osteltamivir is supposed to double by the end of this year, and the federal government intends to purchase another 20 million, Hayden says. But with our population at close to 300 million and a pandemic’s estimated attack rate of 30 percent, we need enough antiviral medication for 90 million people—a significant shortfall.

—Dr. Frederick Hayden The Miller Center: Sean Gallagher
The Ethics of Rationing
In the event of a pandemic, such shortages raise a host of moral questions, says John Arras, a UVA professor of bioethics and philosophy. As a member of the CDC’s Ethics Advisory Group, Arras is grappling with the tough health-care choices that will have to be made if a pandemic becomes a reality.
“The most obvious questions revolve around the rationing of scarce resources, from antiviral agents and vaccines to available hospital bed space, to access to medical personnel and ventilators,” he says.
The scarcity of a vaccine is a prime example of this ethical dilemma. During a normal flu season, the U.S. and other countries have in past years determined that vaccines go first to the most vulnerable—the aged, the seriously ill, very young children and pregnant women. Recently, the CDC added health-care personnel and people who care for infants to its priority ranking. In a pandemic, however, should social imperatives be considered as well as medical ones? Shouldn’t workers who are essential to societal functioning during crises—vaccine manufacturers; hospital staff; police; firefighters; food production, transportation and utility workers; the president and key government officials—be accorded priority?
There are also related economic concerns, Arras notes. Assessed strictly on a cost-benefit basis, should precious vaccine be accorded to the incapacitated or the unemployable, or should it be reserved first for prime working-age adults? These are heart-wrenching decisions, but a pandemic will necessitate them.
The moral choices facing us are ultimate ones, and Arras says that they all stem from the key question of bioethics: “Who shall live when not all can live?” By way of precedent, Arras recalls the deliberations of the bioethical thinkers who originally grappled with the problem of organ transplantation. A committee of experts, they thought, could decide who would receive organs by evaluating the potential net social contributions of candidates.
Critics, however, vehemently protested. They agreed, Arras says, with moral theologian Paul Ramsey in holding that basing life-and-death judgments on such utilitarian criteria ignores the equal intrinsic worth of every human being. Instead, we should prioritize by random decision procedures—a lottery, perhaps, or by the custom of “first come, first served.” Even Ramsey, however, conceded that in certain crisis situations, assessments of social worth might be permissible. Would a pandemic, Arras wonders, be one of these?
As it stands now, he adds, we have some incompatible policy goals—the protection of the most vulnerable, of health-related personnel, of societal infrastructures, and the achievement of maximal societal utility. He insists that we are seriously overdue in determining fair rationing principles that ensure social functioning without discriminating against the poor and dispossessed. Such a determination, “forged within a context of public democratic deliberation,” Arras says, must become a national priority.
An Economic Catastrophe
To begin assessing the economic impact of a pandemic, Peter Rodriguez, a Darden School professor of business administration and a specialist in global economies and markets, reviews the 1918 case. “It struck, as AIDS now does, a prime working-age population, a very large number of 15- to 54-year-olds. That meant that our ability to provide resources, even to handle or mitigate the effects, or to support the deficits, taxes and spending that go along with trying to rein in some of the devastation, was severely damaged.”
These days, with the economy “running at massive fiscal strain,” he says, a pandemic could spell disaster.
“With the extraordinary health-care costs that would ensue,” Rodriguez says, “it’s possible that the strains on our federal budget would be too much to handle without a relatively dramatic shift in interest rates or the value of the dollar.” He adds that a pandemic would likely hit urban areas, “where [the gross domestic product] is highly concentrated, and hit those who work in high value-added fields,” a workforce crucial to keeping an economy afloat. During the Great Depression, the nation suffered an enormous loss of talent when so many people lost their jobs. Rodriguez speculates about a similar situation occurring in a pandemic—workers losing jobs temporarily, but perhaps finding their specific jobs phased out when they attempt to return.
He also points out the remarkable costs of economic reconstruction after a disaster. “For example, in the aftermath of [Hurricane] Katrina or 9/11, there was great demand for replenishing all the things we’d lost in order to establish a sense of security. That, in effect, always goes to the bottom line of higher GDP or higher growth—and it’s things that we would be better off if we didn’t have to spend for.”
A pandemic, he says, can defeat the most resilient of markets. Rodriguez’s study of development economics in nations that have been severely damaged by disease convinces him that “it really takes great leadership and preparedness. It’s not just a matter of having the market in place. In New Orleans, we found that we had a hard time getting things done. If you look at something on the scale of a pandemic, maybe the thought of the economic implications of it are just too scary for most of us.”
But not everyone feels that 1918 points to an inevitable pandemic, or a similar outcome should one occur. UVA history professor Duane Osheim, whose field of study is the plague and epidemic disease in Renaissance Europe, in fact cautions against too ready a comparison to the early-20th-century outbreak. History never repeats itself exactly, he says. “Don’t we move around more now? Isn’t our housing different, our sense of hygiene?” he asks. And because we’ve changed, so will our culture react to a pandemic in its own way. We may share with citizens of the past a fear of the unknown, Osheim adds, but it’s a fear that information may help to quell.
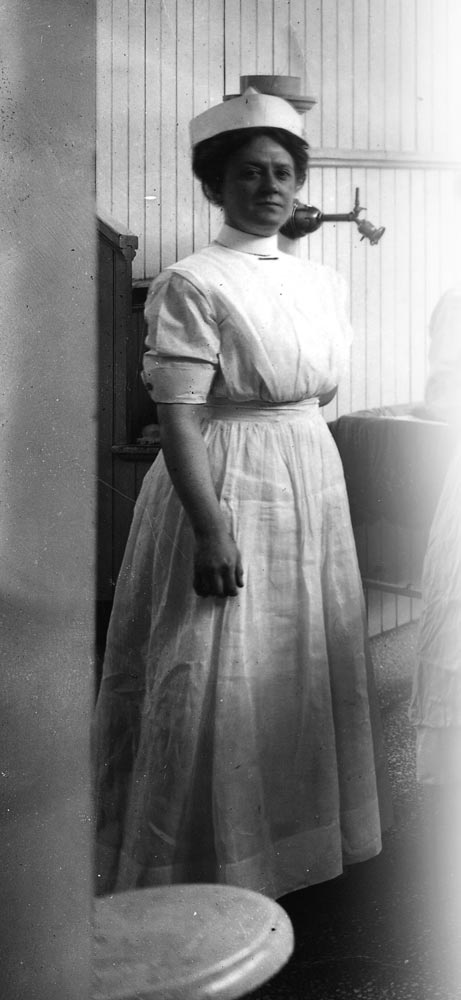
At UVA, the 1918 outbreak of Spanish influenza warrants just two sentences in Virginius Dabney’s exhaustive Mr. Jefferson’s University: “During the dreadful influenza epidemic in the fall of 1918 all students wore white masks, in the hope of avoiding the deadly pestilence. Many fell ill and some died, including able Prof. William Harry Heck, who was lecturing on how to avoid the flu.” In St. Denis, France, UVA’s Base Hospital 41 struggled to cope with the sudden influx of flu patients, which peaked in October 1918: “Twenty-five percent of the officers, nurses and enlisted men were in the hospital with influenza; we had over 2,000 patients, and word came then that 700 more were on the way ... the figures are staggering,” a correspondent reported in the May 1919 issue of UVA Alumni News.
The Charlottesville Daily Progress—itself forced to scale back production and delivery because of a flu-induced worker shortage—documented the flu’s local impact. Besides numerous obituaries, many for relatively young citizens, there was a proclamation from the mayor temporarily closing “schools, public and private, churches, theatres, and all other places where there are public congregations” to slow the disease’s spread, and an appeal from the Albemarle Telephone Company to limit calls, due to a lack of healthy operators.
The U.S. surgeon general, Rupert Blue, issued warnings against contact with bodily fluids, and admonitions to safeguard oneself by maintaining “a proper proportion of work, play and rest, by keeping the body well clothed, and by eating sufficient wholesome and properly selected food,” especially milk. “Make every possible effort to breathe as much pure air as possible,” he added.
Advertisers offered myriad flu remedies, including Vick’s VapoRub, Dover’s powder and Foley’s Honey and Tar. But Blue warned against over-the-counter cures: “It is foolish to ask the druggist to prescribe and may be dangerous to take the so-called ‘safe, sure and harmless’ remedies advertised by patent medicine manufacturers.”
Finally, after weeks of bad news, the Progress began sprinkling in a few brief-but-hopeful social notes. “The many friends of Miss Nellie R. Burgess will be glad to know she is able to be out again after being very ill with Spanish influenza,” it reported.

