What’s Up, Doc?
The human body is a complex machine of about 10 trillion interconnected cells. When we’re healthy, they work together seamlessly and elegantly, but things can go awry in many different ways. It’s little wonder that medical research at the University of Virginia Health System is so diverse. Researchers, doctors and epidemiologists are working with new technology to keep everything from our brains to our blood sugar in good shape.
Scalpel-Free Brain Surgery

Brain surgery is usually an invasive procedure that involves drilling a hole in the skull.
UVA’s Dr. Jeffrey Elias is using focused sound waves to treat patients’ tremors during a scalpel-free surgery deep in the brain. “It proved we could treat deep in the brain with no incisions, no holes in the skull, on an awake patient ... And anyone would believe if you can do that, you can treat other organs [with a similar technique],” says Dr. Neal F. Kassell, founder and chair of the board to the Focused Ultrasound Surgery Foundation.
Elias uses Insightec’s Transcranial Exablate System, a focused ultrasound machine with MRI capability that allows him to look inside his patients’ brains to see the effect of the treatment in real time.
Billy R. Williams, 74, was the first of 15 patients treated by Elias during a clinical trial and was, until the surgery, losing the ability to feed himself or write due to tremors in his hands. He saw immediate results. “I can tee up my golf ball,” he said. “Work a crossword puzzle with one hand. I can do just about anything.”
Artificial Pancreas
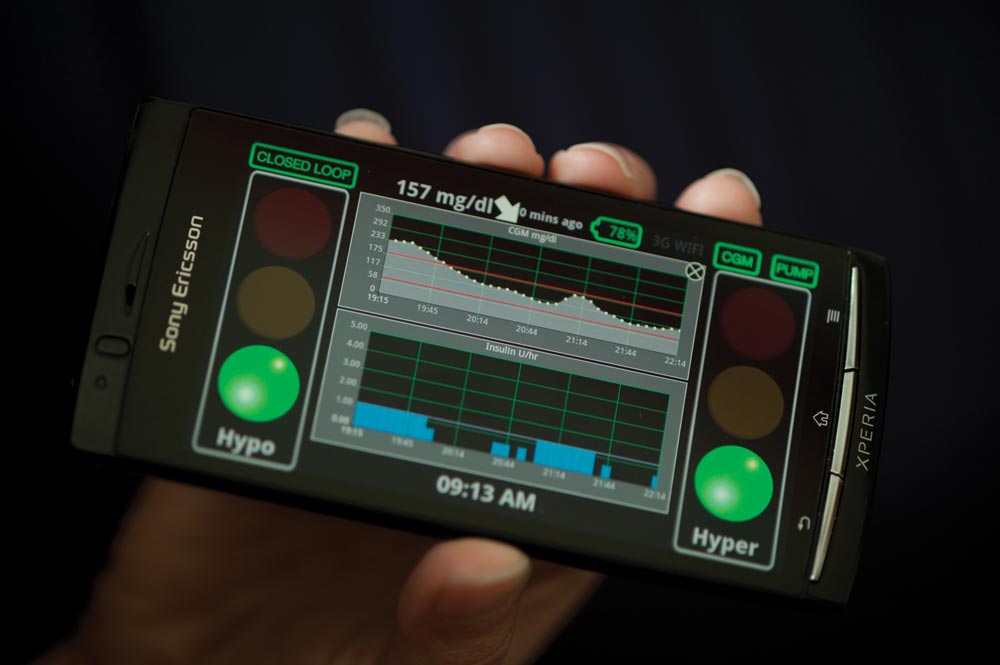
For Type I diabetes patients, maintaining safe blood-sugar levels can be a pain. UVA researchers have developed a novel software algorithm that simulates a healthy pancreas, which has the potential to make life easier for those with diabetes. For the first time, patients have been able to use, in a real-life setting, a hand-held device that automatically delivers insulin to maintain glucose levels.
In the outpatient study, which was conducted in France and Italy, patients with Type 1 diabetes attained near-normal glucose levels after spending a night outside of a hospital while using the artificial pancreas system. The patients were able to eat a restaurant meal and spend one night at a hotel while using the device.
“The success in an outpatient, real-world setting is an enormous and encouraging milestone,” says Boris Kovatchev, professor of psychiatry and behavioral sciences and director of the UVA Center for Diabetes Technology. He and psychiatry professor Patrick Keith-Hynes led the UVA research team.
Tracking Killer Bacteria
On CSI, the police often use DNA evidence to track a murder suspect. UVA researchers are tracing genes to track antibiotic-resistant “superbugs.” Unlike humans, bacteria can give genes to other bacteria; thus bacteria DNA can change quickly. Some genes, including Klebsiella pneumoniae carbapenemase (KPC), can transform regular bacteria into a superbug. Researchers have developed a method of tracking genes like KPC that takes only one to two days and can be performed by most microbiology laboratories. This is much faster and easier than traditional methods. UVA Medical Center epidemiologist Dr. Costi Sifri is the study’s principal investigator.
“We developed and successfully used a novel technique to rapidly track the gene’s movement between patients and bacteria,” says lead author Dr. Amy Mathers, assistant professor in the UVA School of Medicine’s division of infectious diseases and international health. “We were able to show that all cases in a cluster of hospital infections could be traced back to a single patient. Most cases were linked by movement of the KPC gene between different bacteria.”
On a cop show, first an investigator tracks a killer, then makes an arrest. The research team hopes to follow suit by developing new strategies and tools to prevent the spread of highly resistant bacteria.

